PCT-Guided Antibiotic Therapy

Lower respiratory tract infections can present in many different ways, including acute bronchitis, community-acquired pneumonia, and acute exacerbation of chronic obstructive pulmonary disease.
In the past, this ambiguity was met with almost-automatic antibiotic therapy. Today, we have better information and better ways to decide if antibiotics are warranted.
For More
Information
Procalcitonin (PCT) provides critical biomarker information. PCT is produced by numerous organs at a cellular level after bacterial pro-inflammatory stimulation.1,2
Procalcitonin is a host response to bacterial insult.3-5
Viral Infections inhibit PCT expression, enhancing the ability to distinguish bacterial infections from non-bacterial infections (PCT is not specifically indicated as a viral marker).
- Bacterial infection stimulates PCT
- Viral infection blocks PCT
PCT Algorithm
Lower Respiratory Tract Infections (LTRI): PCT-Guided Therapy
LRTI Antibiotic Initiation Algorithm
For patients with suspected or confirmed lower respiratory tract infection (LRTI), defined as community-acquired pneumonia (CAP), acute bronchitis, and acute exacerbation of chronic obstructive pulmonary disease (AECOPD).
| PCT Value | <0.1 ng/mL | 0.1 - 0.25 ng/mL | 0.26 - 0.5 ng/mL | >0.5 ng/mL |
| Initiation of Antibiotic Use Recommendation | Strongly Discourage | Discourage | Encourage | Strongly Encourage |
| Clinical Considerations |
|
|
||
LRTI Antibiotic Discontinuation Algorithm
| LRTI | ||
| PCT Value | <0.25 ng/mL | ↓ >80% from peak |
| Discontinuation of Antibiotic Use Recommendation | Encourage | |
| Clinical Considerations |
|
|
PCT-Guided Antibiotic Therapy is Safe and Effective for Patients
Significant reduction in antibiotic initiation
- 19% reduction in relative antibiotic initiation in all patients
- 39% reduction in initiation of antibiotics in ED patients
Significant reduction in exposure to antibiotics
- 38% reduction in overall antibiotic exposure for inpatients
- 51% reduction in overall antibiotic exposure for patients in ED
No adverse safety signals associated with PCT guidance for LRTI
- No signal for increase in 30-day mortality, complications or length of stay
Sepsis: PCT-Guided Antibiotic Therapy
For more information, please see full package insert for VIDAS B•R•A•H•M•S PCT (30450-01).
In conjunction with clinical assessments, use of PCT can increase accuracy of early diagnosis and enable more appropriate clinical decisions.
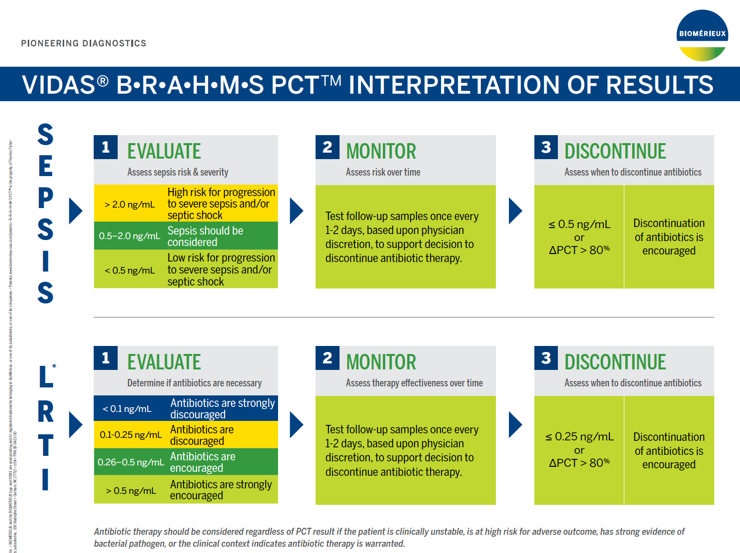
1. Evaluate: Assess Sepsis Risk & Severity
In just 20 minutes, you can get results from a proven, sensitive biomarker that provides specific information that adds to physician acumen, and enables more appropriate triage decisions.
| >2.0 ng/mL | High risk for progression to severe sepsis and/or septic shock |
| 0.5 - 2.0 ng/mL | Sepsis should be considered |
| <0.5 ng/mL | Low risk for progression to severe sepsis and/or septic shock |
2. Monitor: Assess Risk Over Time
Assessing PCT values over time provides valuable information regarding patient disposition, response to treatment, and likelihood of survival.
Follow up samples should be tested once every 1-2 days, based upon physician discretion to support decision to discontinue antibiotic therapy.
3. Discontinue: Assess When to Discontinue Antibiotics
VIDAS B•R•A•H•M•S PCT has been cleared by the FDA to aid in decision making on antibiotic discontinuation for patients with suspected or confirmed sepsis.
Discontinuation of antibiotics is encouraged if the PCT concentration is ≤0.50 ng/mL or if the ∆PCT >80%.
Antibiotic therapy may be continued based upon other clinical findings, such as failure to control a local infection, or ongoing physiologic instability.
PCT is an Important Part of the Solution
For Critically Ill Patients:
- Antibiotic therapy is of great importance
- Prolonged duration is associated with development of antimicrobial resistance
- PCT-guided antibiotic therapy reduces antibiotic exposure and patient length of stay (a 23% reduction in antibiotic exposure)
- No adverse safety signals associated with PCT-guided antibiotic therapy for sepsis
PCT & Antibiotic Stewardship
- Monitor PCT levels
- Gain needed data to make better, more informed decisions
- Additional guidance for initiation and discontinuation of antibiotic therapy
- Improve prescribing practices to slow rise of resistant bacteria
- Support CMS guidelines for antibiotic stewardship and infection prevention
So you can achieve the goal of giving antibiotics to the right patients, at the right time, for the right duration.
Useful Material for Interpreting PCT Results
Clinical Guide to Use of Procalcitonin
VIDAS B•R•A•M•H•S PCT Wall Chart
Learn More About VIDAS® B•R•A•H•M•S PCT™
VIDAS® 3 is a benchtop immunoassay system designed specifically for low throughput testing. Fully automated, it is based on the proven and robust ELFA technology that makes VIDAS a gold standard worldwide for high quality on-demand test results.
- Full traceability
- Specialty menu available in single-test ready-to-use format
- Bidirectional connectivity to internal and external networks
Visit VIDAS B•R•A•H•M•S PCT |
Visit VIDAS 3 |
Order Online |
References: